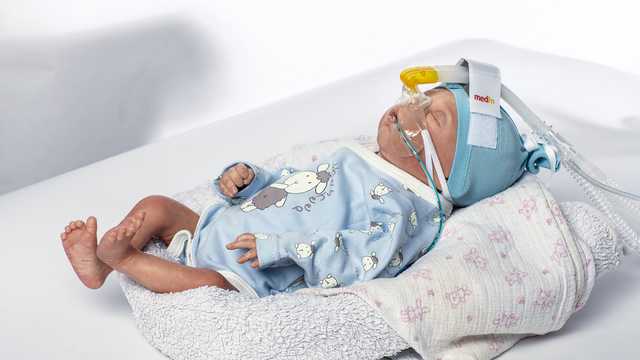
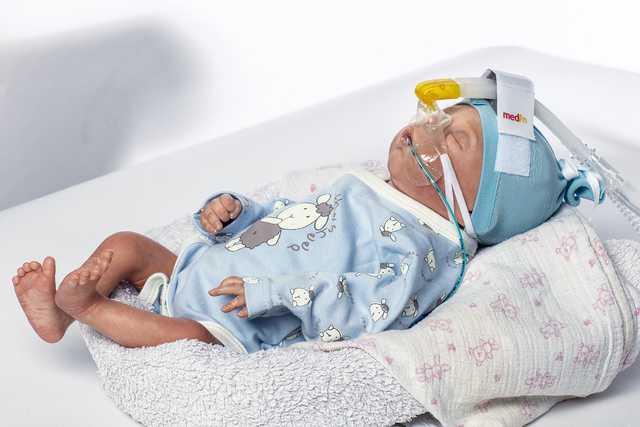
nCPAP (nasal Continuous Positive Airway Pressure, nasaler kontinuierlicher positiver Atemwegsdruck) ist der am häufigsten verwendete Modus der nichtinvasiven Atemunterstützung bei Früh- und Neugeborenen sowie die Grundlage für mehrere weitere Varianten wie NIPPV, SNIPPV und nHFV. Beim Einsatz von nCPAP muss der Patient in der Lage sein, spontan zu atmen, da keine Atemhübe verabreicht werden.
Der wichtigste Parameter bei der nCPAP-Therapie ist der PEEP (positiver endexspiratorischer Atemwegsdruck), der den Druck am Ende der Ausatmung beschreibt.
Bei der Spontanatmung ohne nCPAP können die Inspirationsdrücke in einigen Fällen negative Werte in den Atemwegen erreichen. Mit nCPAP kann der gesamte Atemzyklus des Patienten &ndash sowohl Inspiration als auch Exspiration &ndash auf einem positiven Druckniveau gehalten werden.
Verbesserung der Oxygenierung
Verhinderung eines Alveolarkollapses
Verringerung der Atembemühungen
Aufrechterhaltung der funktionellen Residualkapazität
Stabilisierung der Atemwege (
medinCNO, medinCNOmini und medin-NC3 bieten nCPAP in Kombination mit erweiterten Modi wie ApnoeCPAP, NIPPV, SNIPPV oder nHFV. Unsere Geräte EasyBlender, BubbleCPAP und medinSINDI arbeiten ausschließlich mit nCPAP.
Neben diesen speziellen nCPAP-Geräten können auch viele Beatmungsgeräte &ndash zum Beispiel Hamilton Medical Geräte &ndash verwendet werden.
Allen Varianten ist gemeinsam, dass sie durch die Interaktion zwischen Atemgasflow und definierten Widerständen einen Druck im Atemweg des Patienten aufbauen. Der Typ des nasalen Interface spielt hierbei eine wichtige Rolle.

Das nCPAP-Interface (Miniflow) wird über einen Inspirations- sowie einen Exspirationsschenkel des Schlauchsystems an ein Beatmungsgerät, eine Driver-Einheit oder an ein BubbleCPAP-System angeschlossen.
Am Ende des Exspirationsschenkels befindet sich ein Ventil, das sich in Abhängigkeit vom gewählten PEEP-Wert öffnet oder schließt. Der im System zirkulierende Gasflow erzeugt den gewünschten Druck an diesem Ventil.
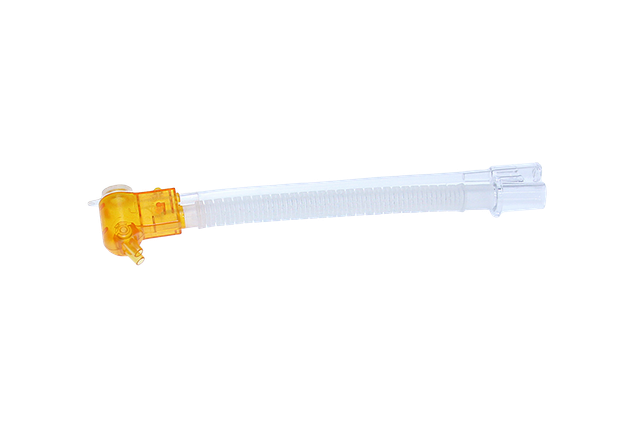
Die nasalen Interfaces dieser Systeme (Medijet) sind mit einem Ventil ausgestattet, das den Druck direkt am Interface in Verbindung mit dem Gasflow erzeugt. Sie werden daher auch häufig als CPAP-Generatoren bezeichnet.
In Kombination mit einem CPAP-Gerät wird üblicherweise ein Schlauchsystem mit nur einem Inspirationsschenkel verwendet.
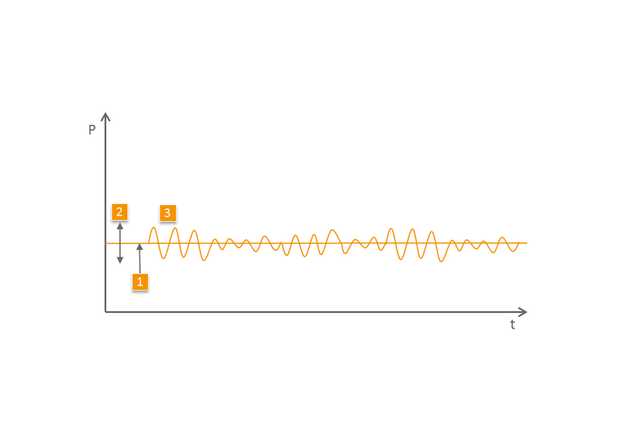
1 PEEP/CPAP
2 Amplitude der Spontanatmung in Bezug auf den PEEP
3 Drucksignal der Spontanatmung