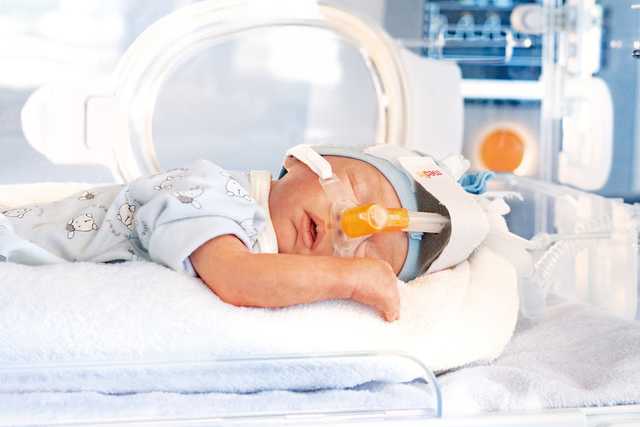
Apnea and breathing irregularities affect nearly every premature infant and newborn. The more premature the infant is, the more markedly apnea occurs. They represent a disruption in the respiratory mechanics as well as respiratory control. The most important feature of the apnea is the intermittent air flow in the patient’s airway.
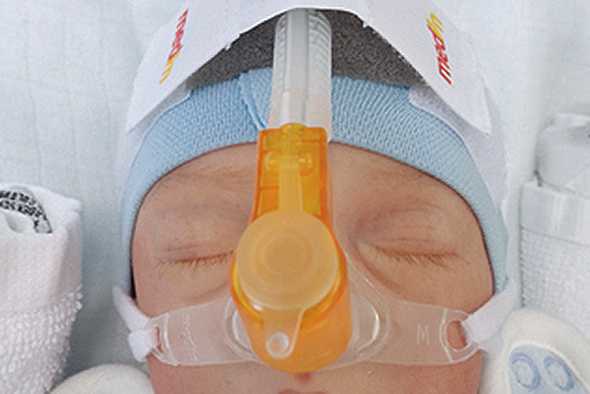
nCPAP (nasal Continuous Positive Airway Pressure) is the most commonly used mode of non-invasive respiratory support in premature infants and newborns as well as the basis for several further variants such as NIPPV, SNIPPV and NHFV. When using nCPAP, the patient must be able to breathe spontaneously, since no breaths are administered.
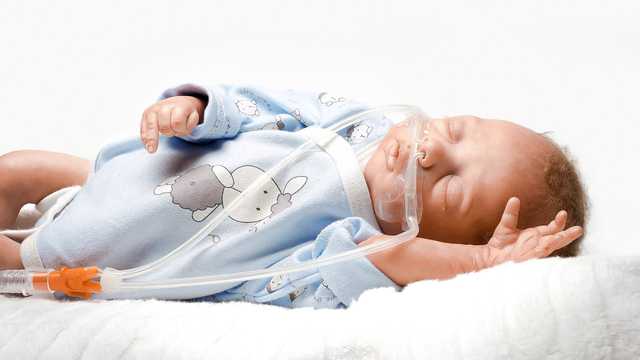
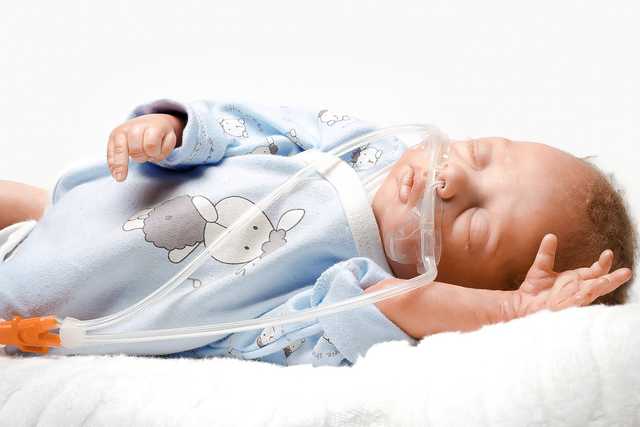
Nasal high-flow therapy (nHFT) describes the supply of heated and humidified breathing gas via a nasal cannula. The gas flow administered is thus higher than the patient’s inspiratory respiratory flow. In neonatology, a flow of more than 1 LPM is considered to be high-flow therapy, while for adults, correspondingly higher values should be applied. (
Other names for nHFT: High-Flow Nasal Cannula (HFNC) or Heated Humidified High-Flow Nasal Cannula. All of them designate the same form of therapy.
nHFV combines the benefits of high‑frequency ventilation and non‑invasive CPAP support (
The umbrella term NIPPV includes modes in which - in addition to CPAP/PEEP - controlled breaths are applied to support the patient. These breaths have a higher pressure level and are not emitted in a synchronized manner. A differentiation is made between the different variants of this form of respiratory support.
SNIPPV is the synchronized variant of NIPPV respiratory support. In NIPPV, the breaths are administered by the device independent of the patient’s own breathing. This can lead to conflicts in the synchronization between the patient and the device. In SNIPPV, the breaths are coordinated to the patient’s inspiration and conflicts are minimized.

Breathing gas conditioning refers to the heating and humidification of the inspired air or the breathing gas administered. This can be done either actively using a humidifier or passively with an HME filter (heat and moisture exchanger).
Since the respiratory system of premature infants and newborns is frequently not yet fully developed or is at least very sensitive, active humidification systems are preferably used for small patients.